Suggestions
Use up and down arrows to review and enter to select.Please wait while we process your payment
If you don't see it, please check your spam folder. Sometimes it can end up there.
If you don't see it, please check your spam folder. Sometimes it can end up there.
Please wait while we process your payment

By signing up you agree to our terms and privacy policy.
Don’t have an account? Subscribe now
Create Your Account
Sign up for your FREE 7-day trial
Already have an account? Log in
Your Email
Choose Your Plan
Individual
Group Discount
Save over 50% with a SparkNotes PLUS Annual Plan!
 payment page
payment page
Purchasing SparkNotes PLUS for a group?
Get Annual Plans at a discount when you buy 2 or more!
Price
$24.99 $18.74 /subscription + tax
Subtotal $37.48 + tax
Save 25% on 2-49 accounts
Save 30% on 50-99 accounts
Want 100 or more? Contact us for a customized plan.
 payment page
payment page
Your Plan
Payment Details
Payment Summary
SparkNotes Plus
You'll be billed after your free trial ends.
7-Day Free Trial
Not Applicable
Renews May 3, 2024 April 26, 2024
Discounts (applied to next billing)
DUE NOW
US $0.00
SNPLUSROCKS20 | 20% Discount
This is not a valid promo code.
Discount Code (one code per order)
SparkNotes PLUS Annual Plan - Group Discount
Qty: 00
SparkNotes Plus subscription is $4.99/month or $24.99/year as selected above. The free trial period is the first 7 days of your subscription. TO CANCEL YOUR SUBSCRIPTION AND AVOID BEING CHARGED, YOU MUST CANCEL BEFORE THE END OF THE FREE TRIAL PERIOD. You may cancel your subscription on your Subscription and Billing page or contact Customer Support at custserv@bn.com. Your subscription will continue automatically once the free trial period is over. Free trial is available to new customers only.
Choose Your Plan
For the next 7 days, you'll have access to awesome PLUS stuff like AP English test prep, No Fear Shakespeare translations and audio, a note-taking tool, personalized dashboard, & much more!
You’ve successfully purchased a group discount. Your group members can use the joining link below to redeem their group membership. You'll also receive an email with the link.
Members will be prompted to log in or create an account to redeem their group membership.
Thanks for creating a SparkNotes account! Continue to start your free trial.
We're sorry, we could not create your account. SparkNotes PLUS is not available in your country. See what countries we’re in.
There was an error creating your account. Please check your payment details and try again.
Please wait while we process your payment

Your PLUS subscription has expired
Please wait while we process your payment
Please wait while we process your payment

Because proteins are a highly evolved and diverse class of molecules, they perform endless tasks and functions within both plants and animals. They are important in the biosyntheses of hormones, enzymes, and membrane channels and pumps. In animals, proteins also function in the immune system and can be used in the production of energy. In essence, proteins are the currency of life.
Since proteins constitute the majority of tissues in the body and since these tissues are constantly in protein flux, proteins are degraded and synthesized within all tissues on a regular basis. Some of the amino acids that are degraded can be recycled by the liver and used again for other biosyntheses, but a significant portion of this protein cannot be replaced.
Through a process known as transamination, the liver synthesizes amino acids.
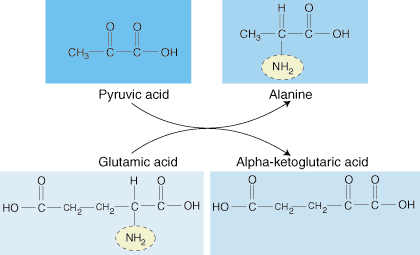
When the body's energy sources are low, it begins to degrade proteins for use as an alternative energy source. Amino acids can be classified as glucogenic or ketogenic.
Glucogenic amino acids can be degraded to pyruvate or an intermediate in the
Krebs Cycle. They are named glucogenic because they can produce glucose
under conditions of low glucose. This process is also known as
gluconeogenesis, or the production of "new glucose." Amino acids form
glucose through degradation to pyruvate or an intermediate in the Krebs Cycle.
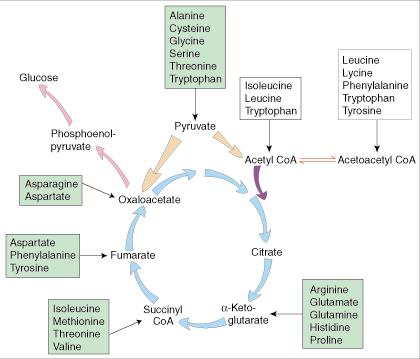
In contrast, ketogenic amino acids can produce ketones when energy sources are low. Some of these amino acids are degraded directly to ketone bodies such as acetoacetate (see ). They include leucine, lysine, phenylalanine, tryptophan, and tyrosine. The other ketogenic amino acids can be converted to acetyl CoA. Acetyl CoA has several different fates, one of which is the conversion to acetoacetate. Although not a preferential energy source, acetoacetate can be metabolized by the brain and muscle for energy when blood glucose is low. Acetoacetate cannot be used in gluconeogenesis, since acetyl CoA cannot be converted directly to oxaloacetate.
Please wait while we process your payment

